Prior Authorization Updates
By TherapyNotes, LLC on October 19, 2022

We have made numerous improvements to prior authorizations to help streamline your workflow. Prior authorizations are now displayed within an insurance policy instead of in a separate section. Therefore, there is no longer a policy dropdown in the Prior Authorization section. We've added functionality to make it easier to add and edit prior authorizations and track their usage and expiration dates. You can now enter authorization codes without specifying a service code, so it will be used with any service, or you can enter multiple service codes for which it applies. In addition, prior authorizations can easily be disabled and prior authorization reports now have additional filters.
Viewing, Adding, and Editing Prior Authorizations
Previously, prior authorizations were added separately from insurance policies, and the appropriate policy was chosen within the prior authorization. With this update, billers will now go to the insurance policy edit screen to add or edit a prior authorization. When adding or editing the prior authorization, there are now additional parameters you can select or enter, including start and expiration dates and usage settings (once per service or per unit). Additional changes include the ability to set service codes to "any", include add-on codes, or set specific service codes. Multiple authorization codes for a single service code for the same time frame may also be added. TherapyNotes will automatically use the older authorization when generating claims.
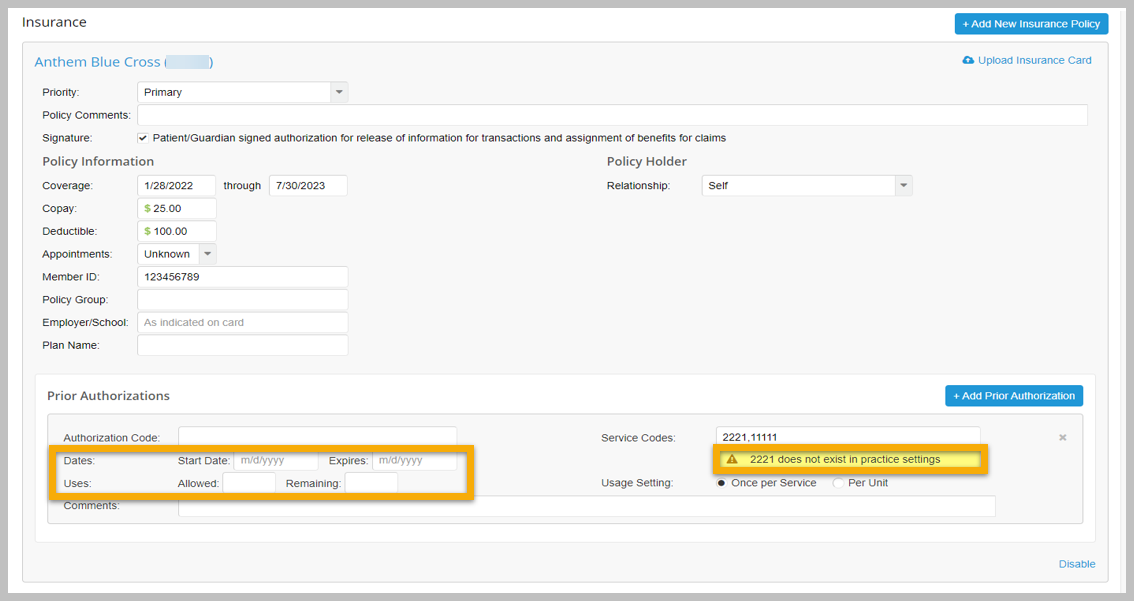
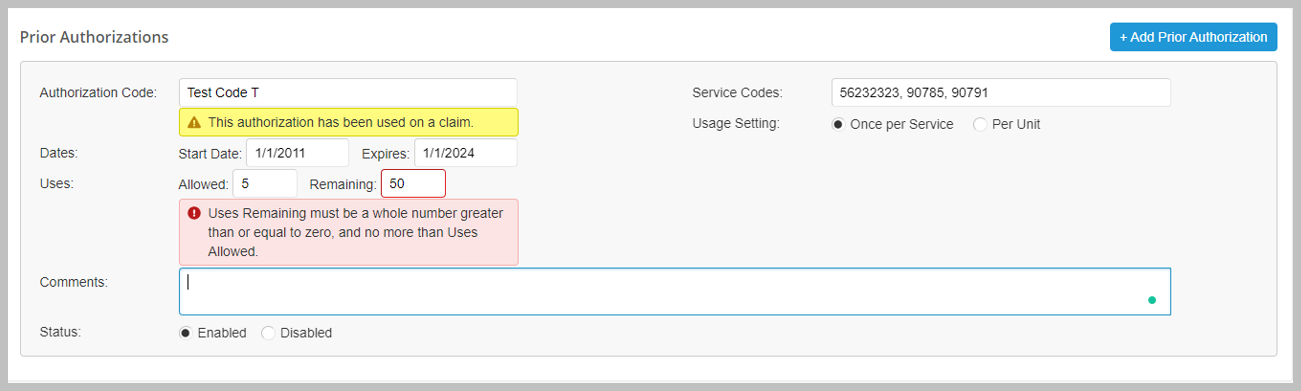
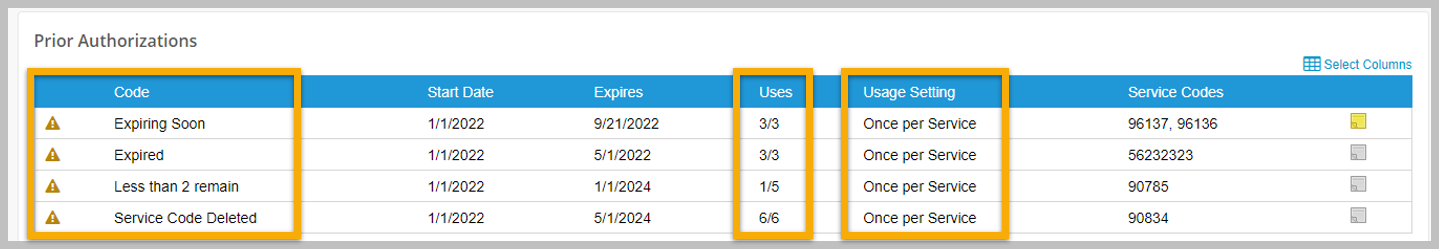
With this update, we have added more warnings to ensure accuracy when adding or editing prior authorizations. Warning messages will appear if the prior authorization contains service codes that do not exist, incorrect values are entered for the number of uses allowed or uses remaining, and if it has been used on a claim. In addition, billers will now see more warnings when viewing prior authorization lists; warning icons will appear next to prior authorizations that have fewer than 2 uses remaining, are expiring soon, have expired, or have deleted service codes. When viewing a claim on the Submit Electronic Claims page, a yellow banner will display showing how many uses are left if the prior authorization for the claim has fewer units remaining than are needed for submission.
Disabling and Deleting Prior Authorizations
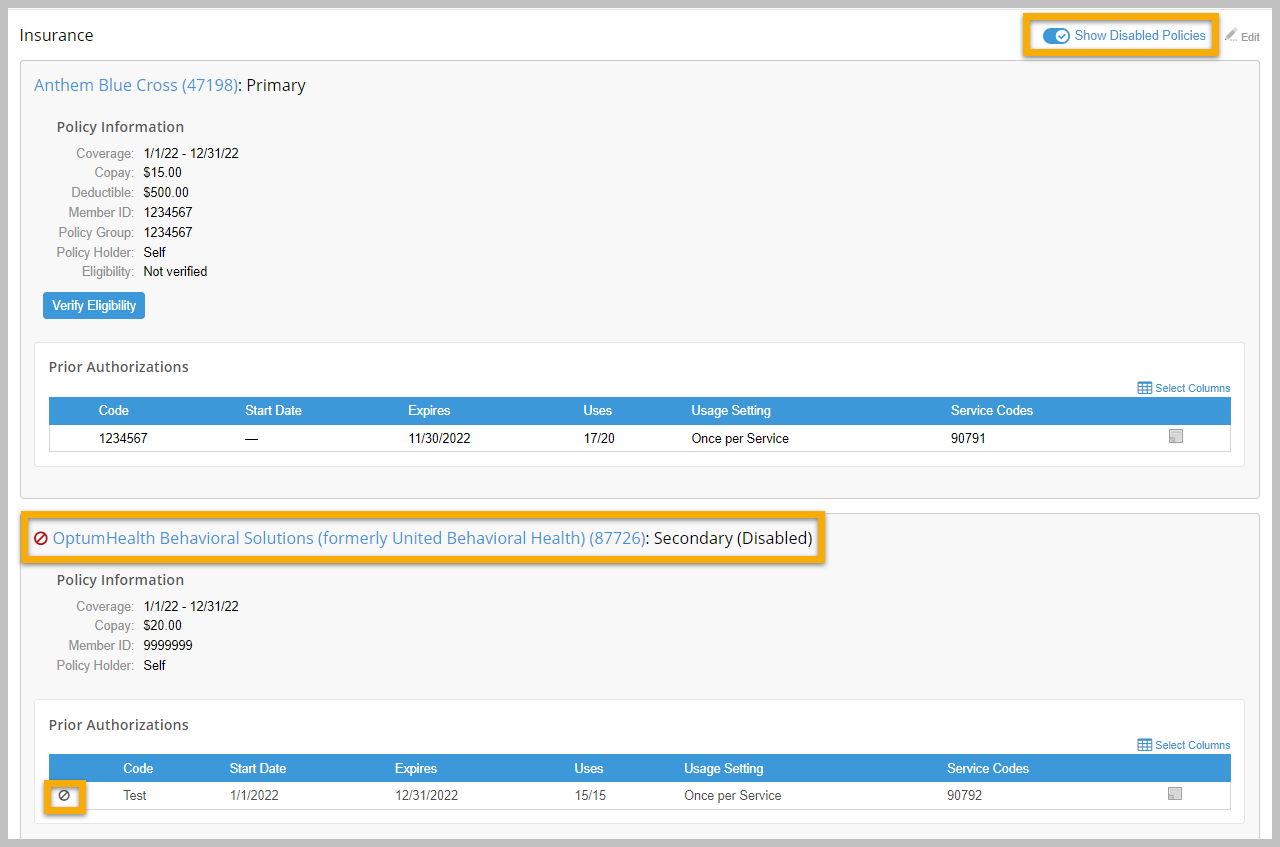
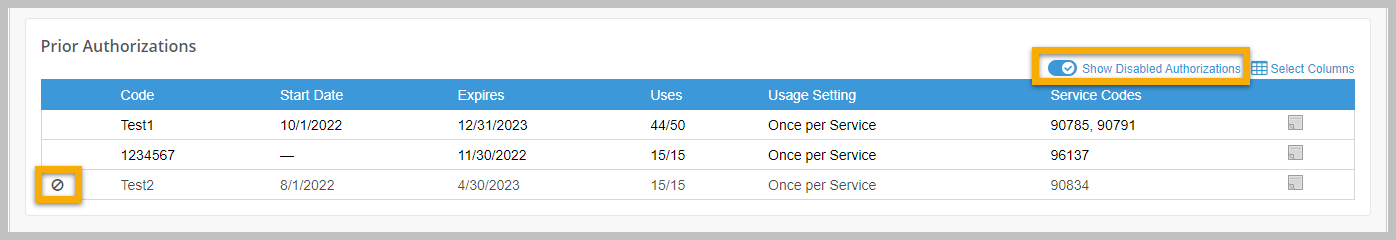
Prior authorizations can now be disabled or deleted. If the prior authorization has been saved and has not been used on a claim, it can be deleted. However, if it has been used on a claim, you can only disable it. Billers also have to ability to view or hide disabled insurance policies and prior authorizations. If you disable an insurance policy, the prior authorizations associated with it will automatically be disabled. Note that if you re-enable a policy, any prior authorization within it will not automatically be enabled; you will have to manually re-enable it.
Prior Authorization Reports
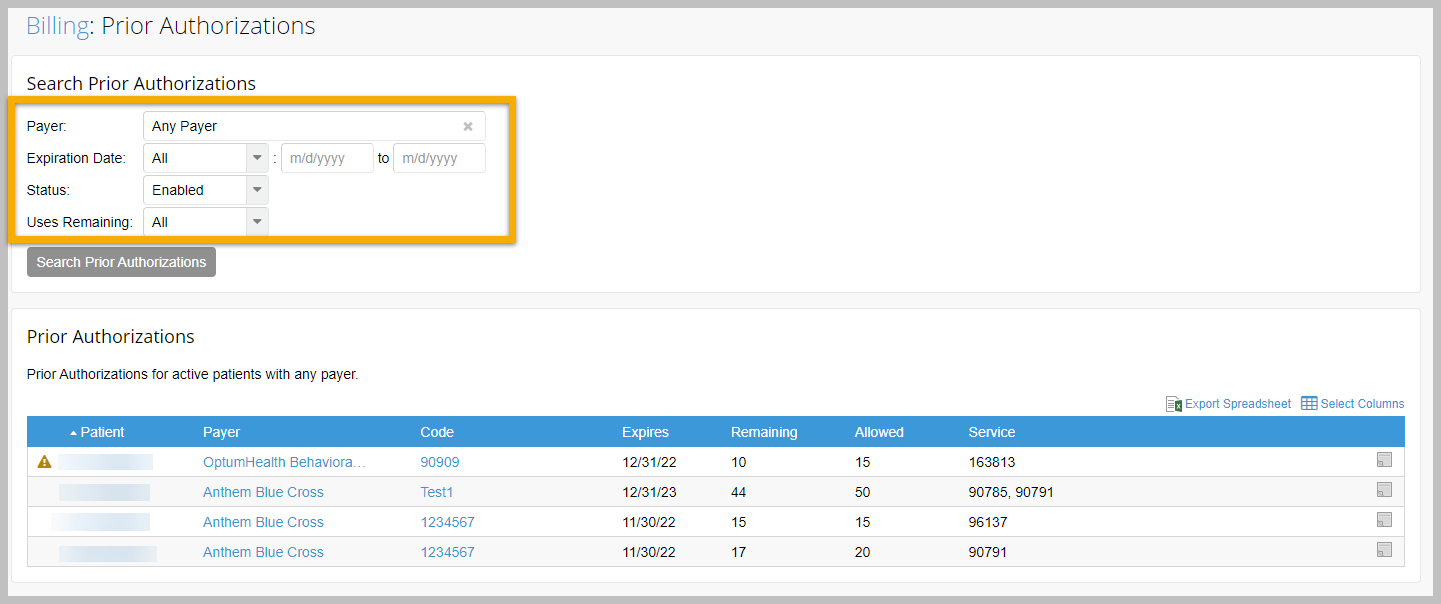
With this update, we have also added to ability to filter prior authorization reports by expiration, date, status, and uses remaining. Previously, these reports could only be filtered by payer. Reports now also display warnings if the prior authorization is expired, if there are no uses remaining, or if one or more service codes do not exist. All columns on the report will be exported when downloaded as an Excel spreadsheet.
* The content of this post is intended to serve as general advice and information. It is not to be taken as legal advice and may not account for all rules and regulations in every jurisdiction. For legal advice, please contact an attorney.
Get more content like this, delivered right to your inbox. Subscribe to our newsletter.
More Content You'll Enjoy
TherapyNotes Achieves HITRUST AI Security Certification for TherapyFuel

What’s New: Messaging Glow Up and Workflow Improvements
